By Lia Butler, Client Experience Specialist
When women picture what their birth experience will look like, we hope for an easy delivery followed by those blissful postpartum days enjoying newfound motherhood. For me, I immediately took myself off the list of people who had complications during pregnancy/delivery. That happens to “other people” and I would not be joining that club. The thing is, we do not get the luxury of choosing to remain off that list. Nobody prepares you for the overwhelming rollercoaster of emotions that come along with a less than perfect birth. Its fear of the unknown, guilt in wondering if you could have done something differently, shame that as a woman you couldn’t carry your child safely to term and so much more.
My first pregnancy was fairly normal all the way up until delivery. Let’s just say my birth plan of a natural, unmedicated, perfect experience did not pan out. My son had other plans that led to a very long labor ending in an emergency c-section before my spinal could take full effect. I felt the surgeons first cut and their hands inside of me but that is when I learned how deep a mother’s love truly is. I did not care about the pain or how traumatic the whole experience was. I just needed for him to be out safely. Jax Butler entered the world yelling at us all for the inconvenience of his quick delivery. He needed to be in the NICU briefly for monitoring but was able to return to me within 24 hours. I felt so relieved that I didn’t have to be a “NICU Mom,” dealing with all the fear and heartache that can come along with it. I told myself that my next birth would be a breeze. I pictured an unmedicated VBAC following a perfect pregnancy.
My second pregnancy was going great until my 20-week anatomy scan. I was informed that my daughters’ stomach was measuring very small, which meant that she was not receiving the appropriate amount of nutrients. This led to twice weekly monitoring with a perinatal specialist and a diagnosis of IUGR (intrauterine growth restriction). Her stomach continued to measure small week after week and they started to toy with the idea of early delivery, with the thinking that she would thrive better on the outside where nutrient delivery could be closely monitored. Again, plans changed when my blood pressure shot up to scary numbers and I found myself with severe preeclampsia. The only cure for this condition is delivery, which happened within an hour of me getting to the hospital. I had not planned to have a baby that day, much less another major abdominal surgery.
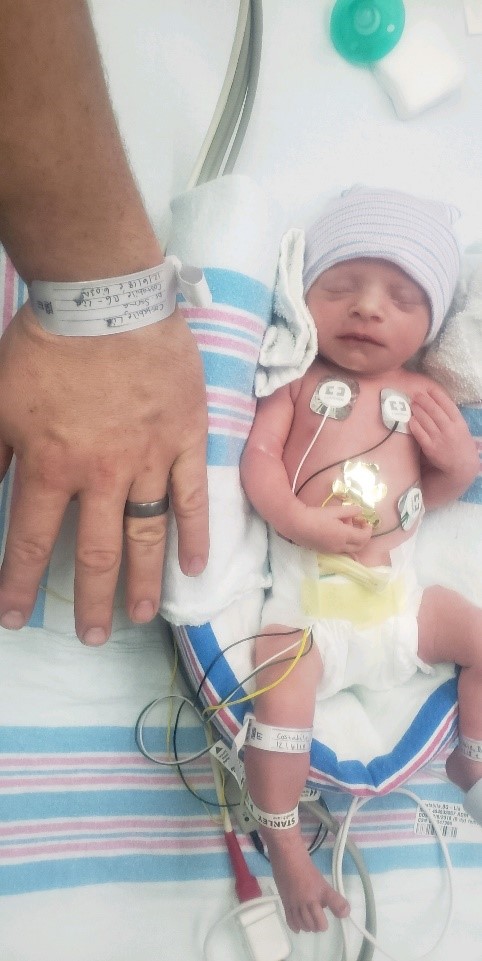
I will never forget laying there in the operating room, petrified, not so patiently waiting to hear that first cry. They took her out and I heard, “Wow she is very small.” It seemed like an eternity before I heard any sounds of life. The nurse walked over to us and said, “Your baby is okay, but she is struggling to breathe. We are taking her to the NICU.” We got to see her for 10 seconds before they whisked her away, and there I was feeling totally helpless. The neonatologist who performed the initial assessment on Rae in the OR said that my having preeclampsia was a blessing because my placenta was dying, and if we waited much longer to take the baby out there would have been a very different outcome.
It is so counterintuitive to be separated from your newborn baby. Nature kicks in and demands that you hold, feed, snuggle and cherish this new being you spent so much time growing and loving. After twelve hours I was finally able to be wheeled into the NICU to see Rae who was being fed my pumped breastmilk, by a stranger. She was crying and refusing the rubber nipple and I could tell she just wanted her mother. I wanted to jump across the room and steal her back, but we were stuck there and I had no choice in the matter. The attending neonatologist was there letting me know of the care plan. I do not remember much from that conversation because I was still on Magnesium, which is a medication to prevent seizures for mothers experiencing preeclampsia. Magnesium makes you feel drunk, so I certainly was not in a place to process all the information that was coming at me. It was a jumbled mix of mentions of feeding tubes, concern for irregular breathing, low blood sugars, etc. I was overwhelmed and felt inadequate for not having the slightest clue on how to take care of my own baby. I was lucky to have a good support system that helped guide me through the difficult process.
My husband was supportive and encouraging despite his own emotional rollercoaster he was riding. The doctors were knowledgeable and kind, taking their time to make sure I was confident in their treatment plan and fully understood what was happening. Then there were the countless nurses who I am forever grateful for. If it wasn’t for their help and support, I don’t know how I would have gotten through. Not only did they take impeccable care of my baby, but they wiped away my tears, emptied my foley bag, helped me learn to breastfeed a preemie, acted calmly when scary situations arose, etc. At one point I was doing skin to skin with Rae and all the alarms started going off. Rae was a dusky grey color and her oxygen saturation had dipped pretty low. The nurse calmly walked over and took her to the isolette. She suctioned and repositioned her a few times and before I knew it, her color had returned and her saturation came up to normal levels. The nurse’s calmness kept me from absolute panic, and it amazed me that she was capable of saving these tiny humans from scary situations time and again without a break in stride.

Despite my best efforts, I became a NICU Mom and have had to understand the hardships that go along with it. As part of the Astarte Medical team, I am able to contribute to lessening those hardships that other families have to endure in the NICU. It is cathartic and rewarding and I am truly honored to be part of a company that dedicates its time and resources to improving the lives of the tiniest, most vulnerable patients.